VeraSTAT-Sports Performance
VeraSTAT-Sports Performance
Best in the Field
![Running Man Vector Green [Converted]](https://www.randox.com/wp-content/uploads/2023/02/Running-Man-Vector-Green-Converted-1024x707.png)
VeraSTAT-Improve your performance
As the best it’s field, the Randox VeraSTAT device allows athletes to overcome the limitations of other generation tests, providing accurate, cost effective and reliable results that will help users receive the care necessary to get them back on their feet and back to their best.
Monitoring response to exercise is vitally important to an athlete and trainer. While a heavy training schedule can lead to chronic immunosuppression in athletes, it is essential that they receive the appropriate care in the case of a dip in health state. Eliminating the risk of inflammation and infection is essential to preventing disruptions to practice and performance.
VeraSTAT Test Menu
The VeraSTAT testing menu is designed to monitor an athletes immune response to exercise. C-Reactive Protein (CRP) levels are used to guide the treatment of bacterial infections or inflammation associated with tissue injury and other inflammatory disorders. On the other hand, Mxyovirus Resistance Protein 1 (MxA) is used as a key indicator of viral infections. These tests used in combination, can allow healthcare clinicians to determine the best course of treatment and get the athlete back to full health
C-Reactive Protein (CRP)
CRP is a Key indicator of inflammation and stress, often resulting from the breakdown in tissues. Overtraining can lead to elevated levels of CRP in the body.
Myxovirus Resistance Protein I (MxA)
MxA is a key indicator of a viral infection which may impact physical performance and activity levels. Unexplained failures are often attributed to recent or current infections.
CRP Assay
Reagent | C-Reactive Protein (CRP)
C-Reactive Protein (CRP): The Most Sensitive Acute Phase Reactant
Benefits of the Randox Assay

Limited Interference
The Randox CRP assay has shown to have limited interference from conjugate and free bilirubin, haemoglobin, Intralipid® and triglycerides.

Liquid ready-to-use
The Randox CRP assay is available in a liquid ready-to-use format for convenience and ease-of-use.

Stable to expiry
The Randox CRP assay is stable to expiry when stored at +2oC to +8oC.

Applications available
Applications available detailing instrument-specific settings for the convenient use of the Randox CRP assay on a variety of clinical chemistry analysers.

Dedicated calibrator and controls available
Dedicated CRP calibrator and controls available offering a complete testing package.
Ordering Information
| Cat No | Size | ||||
|---|---|---|---|---|---|
| CP7950 | R1 7 x 20ml (L) R2 2 x 12ml | Enquire | Kit Insert Request | MSDS | Buy Online |
| CP9742 | R1 6 x 66ml (L) R2 6 x 13ml | Enquire | Kit Insert Request | MSDS | Buy Online |
| CP3826 | R1 6 x 20ml (L) R2 3 x 9ml | Enquire | Kit Insert Request | MSDS | Buy Online |
| (L) Indicates liquid option | |||||
Instrument Specific Applications (ISA’s) are available for a wide range of biochemistry analysers. Contact us to enquire about your specific analyser.
More Information
C-reactive protein (CRP) is the dominant acute phase protein in mammals 1. Elevated levels of CRP are not disease specific but are synthesised, by hepatocytes, in response to pro-inflammatory cytokines during inflammatory and/or infectious processes 2, 3. The physiological function of CRP is the enhancement of cell-mediated immunity through the promotion of phagocytosis, accelerated chemotaxis and the activation of platelets 1.
Known as a biomarker of acute inflammation, many large-scale prospective studies demonstrate the association between CRP and chronic inflammation, including: cardiovascular disease (CVD), cerebrovascular accident (CVA) (ischaemic stroke), Alzheimer’s Disease, and age-related macular degeneration 2.
CRP is a major cardiovascular disease (CVD) risk factor. A CRP level of >10mg/l correlates with a >4% risk of developing a fatal CVD event in 10 years, including: myocardial infarction, peripheral arterial disease, stroke and sudden cardiac death. Inflammation is an integral part in the development and rapid progression of coronary heart disease (CHD) 4.
The coronary artery disease (CAD) process is characterised by increasing levels of inflammatory biomarkers. CRP is not only an excellent biomarker or mediator of atherosclerosis but is a strong independent marker in the prediction of adverse CV events, including: myocardial infarction, ischaemic stroke, and sudden cardiac death. CPR can be utilised as a clinical guide for the diagnosis, management and prognosis of CVD 5.
The development of a cerebrovascular accident (CVA) (stroke) is the result of longstanding vascular inflammation, thrombosis, plaque rupture and subsequent brain ischaemia or infarction. Elevated CRP levels is associated with the development of CVA 6.
High sensitivity CRP (hsCRP) plays an important role in the early diagnosis, prognosis, long and short death risk and prediction of etiological subtypes of stroke 7. Find out more about the Randox hsCRP assay.
Alzheimer’s disease (AD) is the most common form of dementia, accounting for 60-80% of dementia cases 7. CRP is believed to be involved in the pathophysiology of cerebral small vessel disease (CSVD) and neurodegeneration 8. CRP levels are associated with cognitive impairment 9. Inflammation should be considered as a target treatment, with the aim of delaying the progression of subclinical brain damage and cognitive decline 8. Midlife elevations in CRP are associated with an increased risk of developing AD. Patients with AD, CRP elevations continues to predict increased dementia severity suggestive of a possible pro-inflammatory endophenotype in AD 10.
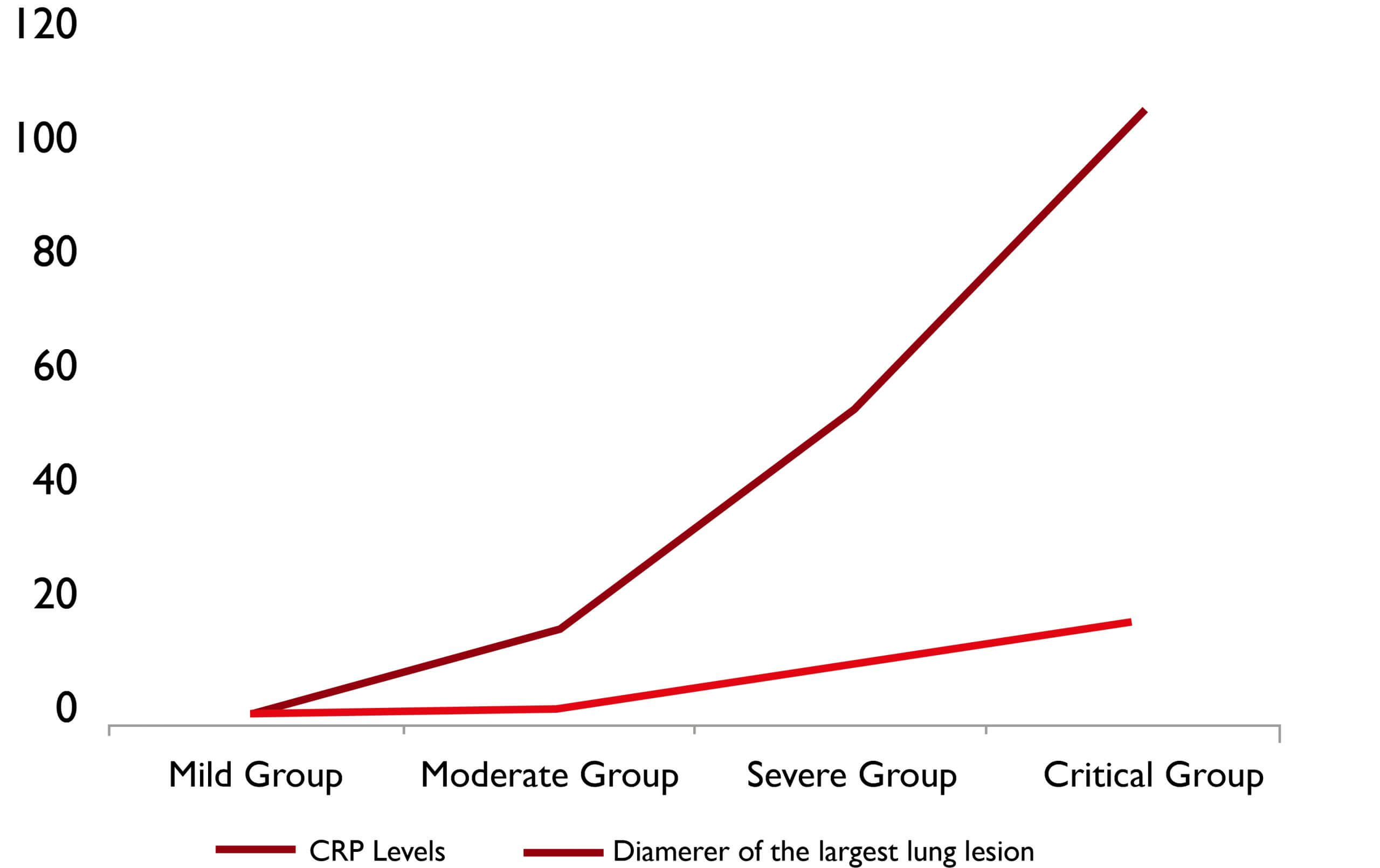
In COVID-19 patients, CRP testing has proved to perform well in discriminating disease severity and predicting adverse outcomes 11. CRP levels positively correlates with lung lesions, reflecting disease severity, and should be considered a key indicator in disease monitoring (see fig. 1) 12.
CRP levels are associated with computed tomography (CT) scores and COVID-19 disease development, with CRP levels increasing in the initial stage of severe COVID-19, prior to the CT findings 13.
Elevated CRP levels have been identified in 86% of patients admitted to hospital. CRP measurements are useful in diagnosis, assessing prognosis and monitoring for clinical improvements or deterioration 14.
Fig. 1. Relation between CRP levels, clinical severity, and lung lesions 12
CRP Calibrator
CRP Control
Specific Protein EQA
Reagents Homepage
References
Inflammatory Biomarker Series: CRP
An inflammatory biomarker detects inflammation in the body. Inflammation is not just the immediate, short-term response of the body to an injury or infection. Inflammation within the body can be a long-term, chronic condition resulting in a number of health implications. In diagnostics, measurement of an inflammatory biomarker can not only detect acute inflammation but provide a marker of treatment response.
C-reactive protein (CRP) is an acute phase protein produced by the liver in response to inflammation, infection and tissue injury. CRP is a particularly beneficial inflammatory biomarker as it is detected much faster than other markers in the blood. Levels of CRP increase when inflammation occurs and therefore it can be a significant biomarker in a range of diseases, including the following.
Cardiovascular Disease
An increasing amount of research exists to suggest CRP is not only a useful, non-specific inflammatory biomarker, but it may have a direct influence on coronary heart disease and cardiac events1. Inflammation can occur when LDL cholesterol builds up in the artery walls causing atherosclerosis. Modifiable risk factors of atherosclerosis include smoking, diabetes, poor diet, high blood pressure and physical inactivity, all factors which subsequently increase the risk of heart attacks, ischemic stroke, peripheral artery disease and even vascular dementia2,3.
Studies have also shown that persistent low levels of CRP can contribute to a person developing CVD. Therefore using high sensitivity CRP as an inflammatory biomarker can detect low levels, helping to predict the likelihood of a patient developing CVD in the future.
Diabetes
Research suggests that inflammation in the body can influence the development of type 2 diabetes. With the ability to be managed through diet and exercise, type 2 diabetes is commonly associated with obesity. Research has shown that excess body fat can cause continuous chronic low-grade inflammation as a result of inflammatory cytokines and increased plasma levels of CRP. As a result, this chronic inflammation has the ability to cause insulin resistance leading to the development of type 2 diabetes4.
Rheumatoid Arthritis
A three year study which analysed the bone and joint health of 10,000 patient samples in India has found that inflammatory biomarkers, in particular CRP and ESR (Erythrocyte Sedimentation Rate) were raised in most of the samples compared to any other markers5. Although CRP is a non-specific inflammatory biomarker, it can be used alongside other tests, such as Rheumatoid Factor, to diagnose inflammatory joint diseases such as Rheumatoid Arthritis. Not only will CRP levels be higher due to chronic inflammation, but CRP levels can be monitored to assess levels of inflammation over time, allowing clinicians offer effective treatment.
Chronic Obstructive Pulmonary Disease (COPD)
COPD is a condition associated with inflammation of the lungs and airways. Studies have shown that measuring CRP levels is beneficial to detect exacerbations, when symptoms of COPD get suddenly worse and can last for several days. This is because CRP levels spike when exacerbations happen, causing lung function to deteriorate6.
Neonatal Bacterial Infections
CRP is one of the preferred and frequently used tests in neonatal units when diagnosing suspected bacterial infections, such as neonatal sepsis, in newborns who show signs on infection. Due to delayed synthesis during the inflammatory response, the sensitivity of CRP is lowest during early stages of infection. It is therefore critical that extremely low levels of CRP can be detected during diagnosis to distinguish whether symptoms are related to an infectious or non-infectious condition. This early detection then allows for rapid and appropriate neonatal treatment7.
Inflammatory Bowel Disease
Research suggests that using CRP as an inflammatory biomarker can help distinguish between Inflammatory Bowel Disorder (IBD) and Irritable Bowel Syndrome (IBS)8. Although IBD and IBS have some similarities in symptoms, IBD causes chronic inflammation, whereas IBS is a non-inflammatory condition. Therefore using CRP as a biomarker can allow clinicians to deliver a confident and accurate diagnosis.
For health professionals
Randox Laboratories manufacture a wide range routine and niche biochemistry reagents for use in both a research and clinical setting. With a wide measuring range, the Randox CRP assay will perform excellently to detect levels outside of the healthy range. Also available is a Full Range CRP assay particularly beneficial for use in a neonatal setting, and a High Sensitivity CRP assay, depending on your diagnostic requirements. For more information, please contact: reagents@randox.com
References:
- Shrivastava, A. K., Singh, H.V., Raizada, A. and Singh, S.K. C-reactive protein, inflammation and coronary heart disease. The Egyptian Heart Journal. 67, 89-97. (2015)
- American Heart Association. Inflammation and Heart Disease. Available from: https://goo.gl/d82Ynr (2016)
- Harvard Health Publications. What you eat can fuel or cool inflammation. Harvard Health Publications. Available from: https://goo.gl/e8m3El (2007)
- Zeyda, M. and Stulnig, T. M. Obesity, Inflammation, and Insulin Resistance – A Mini-Review. Gerontology 2009; 55:379-386 (2009)
- Mukherjeel, R. Bone and joint health are crucial aspect, usually ignored by Indians. The Times of India. Available from: https://goo.gl/qluzhI (2016)
- Anderson, G. P. COPD, asthma and C-reactive protein. European Respiratory Journal 2006; 27: 874-876. (2006)
- Hofer, N., Zacharias, E., Müller, W. and Resch, B. An update on the Use of C-Reactive Protein in Early-Onset Neonatal Sepsis: Current Insights and New Tasks. Neonatology 2012; 102: 25-36 (2012)
- Silva, P. Two Specific Proteins Allow the Exclusion of IBD in Patients with Irritable Bowel Syndrome. IBD News Today. Available from: https://goo.gl/pxMP53 (2015)



